
Operating department practitioner
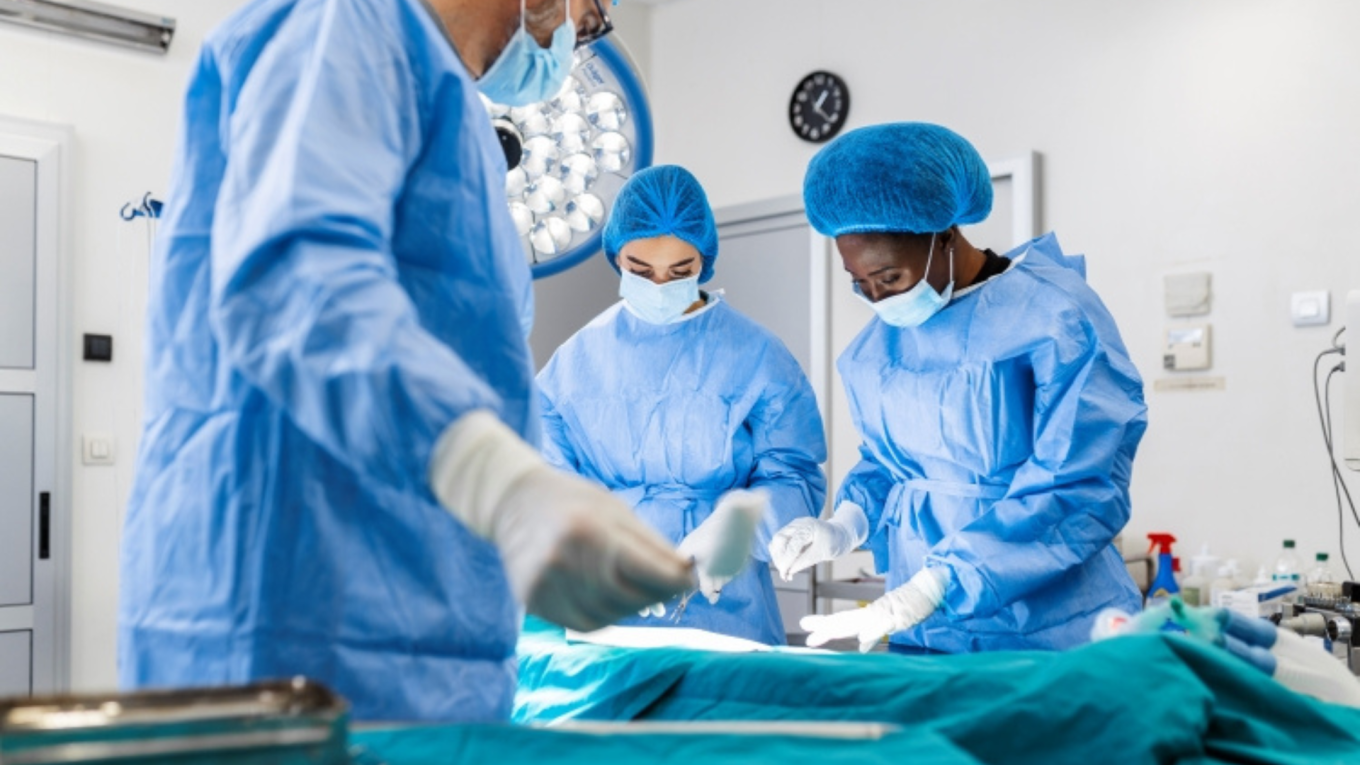
Operating department practitioners (ODPs)* are key members of the surgical team, supporting patients and colleagues through every stage of an operation, from preparation to recovery.
On this page
Introduction to the role
Operating department practitioners (ODPs) are an essential part of the surgical team, providing skilled care and support to patients through every stage of their perioperative journey. This includes the anaesthetic phase, the surgical procedure itself, and recovery.
You’ll work closely with surgeons, anaesthetists, nurses and other theatre staff to make sure everything runs smoothly and safely. This involves preparing operating theatres, ensuring specialist equipment is ready for use, and acting as a vital link between the surgical team and other parts of the theatre and hospital. Your focus will be on patient safety, comfort and wellbeing at all times.
(*ODPs are not recognised as allied health professionals in Scotland.)
About the role
What does an operating department practitioner do?
Operating department practitioners are involved in three main phases of perioperative care: anaesthetic, surgery and recovery. In each stage, your role is to ensure the patient receives safe, skilled and compassionate care, while supporting the surgical team with the specialist knowledge and equipment they need.
During the anaesthetic phase, you will prepare and check specialist equipment and drugs, including anaesthetic machines, intravenous equipment and devices that help maintain a patient’s airway. You’ll also provide reassurance and support to patients before their operation.
In the surgical phase, you will make sure the operating theatre is set up with all the necessary instruments and equipment, from microscopes and lasers to endoscopes. You’ll provide the correct instruments and materials to the surgeon during the procedure, keep track of all surgical equipment and swabs, and communicate between the surgical team and other areas of the hospital. Anticipating the needs of the team and responding quickly is an important part of the role.
In the recovery phase, you will monitor and support patients as they come round from anaesthesia, providing any necessary treatment until they are ready to return to a ward. You will assess their condition carefully to make sure they are recovering safely from the effects of surgery.
What are the pay and conditions like?
If you work as an operating department practitioner in the NHS, you’ll usually have a 37.5 hour working week, which may include some evenings, nights or weekends.
Most ODPs start at band 5 on the Agenda for Change pay scale. You’ll also receive at least 27 days of annual leave plus bank holidays, along with access to the NHS pension scheme and a range of staff discounts.
Where operating department practice can take you
Once you have qualified as an operating department practitioner, there are several ways to progress your career.
You could:
- move into management, education or clinical research
- train to become a surgical care practitioner
- specialise as an advanced critical care practitioner
You’ll have regular professional development reviews to support your goals and keep your skills up to date. You may also choose to join the College of Operating Department Practitioners to access further training, events and networking opportunities.
Working as an operating department practitioner
Working as an operating department practitioner
Person specification
Is operating department practice right for you?
Operating department practitioners work with patients during some of the most important and vulnerable moments of their lives. You’ll need strong communication skills to talk clearly with patients and work effectively with colleagues across the surgical team. Being able to stay focused on safety and noticing small but important details are key parts of the role.
Ask yourself:
- Can I explain information clearly to patients and colleagues?
- Am I confident making decisions that put patient safety first?
Do you have the skills to succeed?
You’ll need excellent observational skills to monitor patients and spot any changes in their condition. Staying calm under pressure and working well with others will help you succeed in a fast-paced and highly skilled environment.
Ask yourself:
- Can I stay focused in a busy clinical setting?
- Am I able to work effectively as part of a close-knit team?
Find a course with UCAS
Want to explore the next step in traditional degree routes into the NHS? Explore courses related to operating department practice with UCAS today.
Entry requirements and training
To become an operating department practitioner, you’ll need to complete a degree in operating department practice at an approved university. Once you’ve successfully completed your degree, you must register with the Health and Care Professions Council before you can begin practising.
You may also be able to train through a degree apprenticeship. This route allows you to earn a salary while gaining your qualification and is offered by some healthcare providers in partnership with universities.
Most universities ask for five GCSEs at grades 4-9 (A- C), including English language, maths and science, along with two or three A levels, usually including a biological science. They may also accept equivalent qualifications such as a BTEC or HND in a science-based subject, a relevant T Level or NVQ, an access to science course, or equivalent Scottish or Irish qualifications.
Every university sets its own entry requirements, so it’s important to check carefully before applying.
Find out more about routes into the NHS with UCAS.
Work experience
Applying for a course or apprenticeship as a operating department practitioner is going to be competitive. If you're seriously considering it, it is a great idea to try and gain some prior work experience to strengthen your application. Visit NHS England to find out more about gaining work experience for careers in the NHS.
Financial support at university
You could receive at least £5,000 a year to help fund your studies while at university in England. Your personal circumstances and the course you choose may mean you could receive more. And the good news? You'll never have to pay it back.
Explore NHS Careers
There are over 350 different NHS careers and everyone makes a difference every day. Whether you’re still in education or thinking about changing careers, you'll get the information you need.